Knee Replacement Exercise Program
- Use ice pack or Game Ready, per instructions for pain 20-30 minutes out of every hour as needed, especially after performing exercises.
- To decrease swelling: Elevate the leg 60 degrees and pump your feet back and forth for 30 minutes. One of the easiest ways to do this is to put your bottom where your pillow is and elevate both legs on your tall headboard. If you don’t have a tall headboard put your feet on the wall behind you..
- NO “Straight Leg Raise” exercises.
- DO NOT place pillows directly under bend of knee, rest instead with pillow under ankle.
- Recumbent bike: Begin 2 weeks after surgery.
- Walk 10 –15 minutes, every hour, during the day.
Exercises for home:
- Ankle Pumps: flexing and extending feet. Try to do 5 minutes per hour while awake
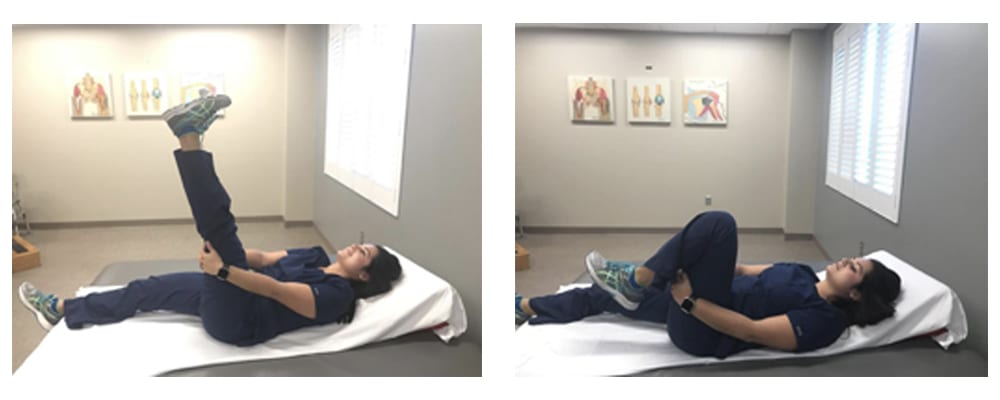
- Knee flexion/extension exercises: Lean back in chair or lie down on bed. Raise operative leg up to your chest and grasp back your thigh with both hands, which are laced together. Now slowly straighten your operative leg and hold 5 seconds. Then let the knee bend with gravity pulling the foot down. Hold for 10 seconds. Do this 3-4 times slowly, 4 times a day.
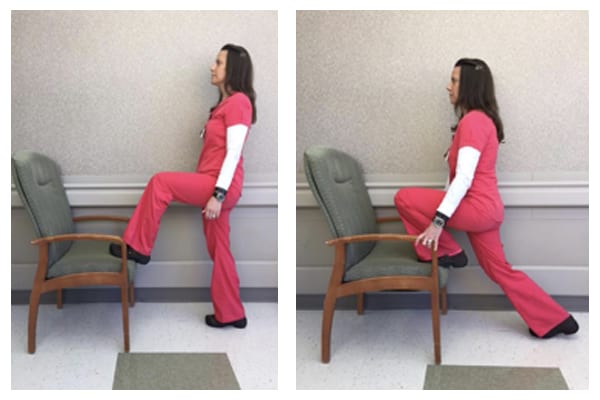
- Knee flex exercises: Sit in a rolling chair with your operative foot up on a stair, stool, or chair with foot flat. Scoot the rolling chair forward, bending the knee until you feel a stretch. Hold for 2-5 minutes. Bend forward a little further holding 2-5 minutes. Repeat these five times, 4 times a day. Progress knee flexion by standing and placing foot of operative leg on seat of chair with arm rest or stairs with rails for stability. Lean forward slowly to bend knee, keeping back straight. Bend forward a little further holding 2-5 minutes. Repeat these five times, 4 times a day. Perform this exercise when you are comfortable with your balance and with supervision.
- Knee flex exercises: Sit in a rolling chair with your operative foot up on a stair, stool, or chair with foot flat. Scoot the rolling chair forward, bending the knee until you feel a stretch. Hold for 2-5 minutes. Bend forward a little further holding 2-5 minutes. Repeat these five times, 4 times a day. Progress knee flexion by standing and placing foot of operative leg on seat of chair with arm rest or stairs with rails for stability. Lean forward slowly to bend knee, keeping back straight. Bend forward a little further holding 2-5 minutes. Repeat these five times, 4 times a day. Perform this exercise when you are comfortable with your balance and with supervision.
Progression 1
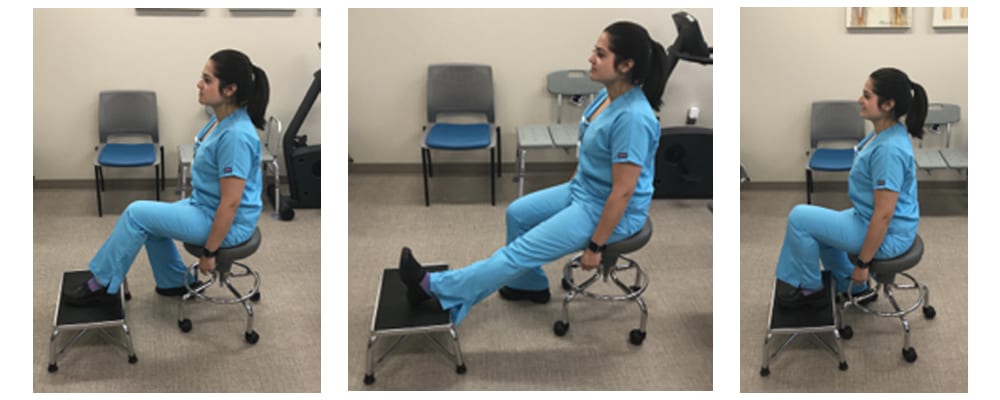
Progression 2

Progression 3
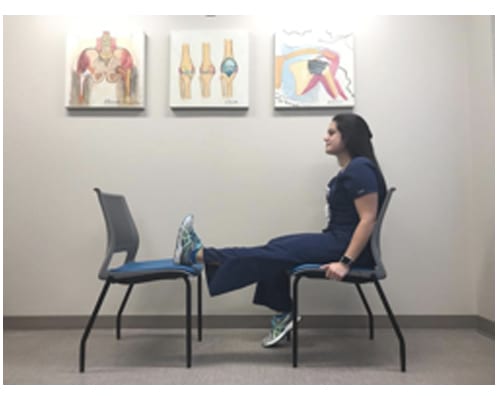
- Chair to Chair Quad Set: Sit in chair and place heel of foot in a chair across from you. Pull toes toward your body. Press the knee down toward the floor by contracting the muscle on top of the leg pushing the knee down hold for 2 minutes. If you have a Game Ready ice machine, use to help decrease pain with this exercise. Do this 3-4 times, three times a day.
- After 2 weeks if you are unable to straighten your knee, you will place a 20 lb. bag of bird seed across the leg to help straighten your knee while doing the chair to chair exercises. Do this for 30 minutes, twice a day.

