Shoulder Arthroplasty

Total Shoulder Arthroplasty / Reverse Shoulder Arthroplasty
Shoulder Anatomy: The shoulder joint is the most flexible joint in the entire human body and is formed by the union of the humerus, the scapula (or shoulder blade), and the clavicle (or collar bone). Along with tendons, ligaments, and muscles, such as the rotator cuff, labrum, biceps, and bursa, they help you reach, swing, and lift in comfort.
Shoulder Replacement: Shoulder Arthroplasty or Reverse Shoulder Arthroplasty is a surgical procedure in which all or part of the glenohumeral joint is replaced by a prosthetic implant. Such joint replacement surgery generally is conducted to relieve severe arthritic pain and fix severe physical joint damage.
Indications: Indications for surgery are persistent pain, instability, trouble lifting, reaching, and inability doing the things you need to do on a daily basis.
Anesthesia: General Anesthesia is given. This means you will be asleep throughout the procedure.
Surgery Time: Approximately forty-five minutes to one hour.
Hospital Stay: You will stay one night in the hospital.
Average Total Recovery Time: Recovery is from two to three months.
Incision: You will have a 4-6-inch incision on the front of your shoulder which will be closed with glue or staples.
Possible Complications: Infection, nerve damage, scar tissue, and anesthesia risk. These happen in less than 1% of the surgeries we have performed.
Normal Post-Operative Occurrences: You will experience bruising, mild to moderate discomfort, swelling and drainage. You may also have an elevated temperature which is normal after any type of surgery. Let us know if your temp is 101 or above and is not brought down with Tylenol. Since we are unable to use a tourniquet you will experience some bruising. It is not unusual to have bruising around the neck, arm, and chest. Icing will help the pain, swelling, and bruising.
Icing after surgery
We highly recommend a Game Ready ice machine for icing your shoulder. It is a machine that has a sleeve that will cover the front and back of your shoulder and is connected to a hose and a reservoir that holds ice and water. Instead of using ice out of the freezer you can freeze 14- 8ox bottles of water and use 7 of them in the reservoir at a time. It helps with pain, bruising, and swelling. It is not covered by insurance and is $100 dollars a week. Your contact person for the Game Ready is Kameron – phone number is 205-269-0200. Call him after scheduling your surgery so he can make sure to set one aside for you. Your shoulder bandage is thick so you will ice a lot during the day and at night for comfort and pain control. After you turn your Game Ready in you may make your own ice bag by mixing 1 cup of rubbing alcohol and 3 cups of water, pouring it into a gallon zip lock bag, and freezing it. It will not get hard, but will be slushy making it easier to cover the front and back of shoulder. This is much colder than regular ice bags.
Dressing: You will have a dressing and a drain in place after surgery. The drain will be removed before you leave the hospital, and your dressing can be removed after 5-7 days or sooner if you have a lot of bleeding. Remove the dressing while in the shower, rinse your incision, pat it dry, then pat it with alcohol, and apply dressing provided by the hospital. You may also cover your incision with 4×4 gauze and tape. This type of dressing is not water proof. You will have staples or glue closing your incision. If he closes with glue you will have a mesh piece of tape on your incision under the dressing. DO NOT remove the mesh tape when changing your dressing in 5- 7 days.
Shower: A shower is allowed 24 hours after surgery unless instructed differently. Leave Silverlon or Mepilex dressing on while showering. Running hot water over your shoulder will help with the pain and with loosening up your joint making it easier to do the simple exercises we give you.
Medications: Your prescription for pain will consist of a pain medication, usually Percocet or Norco. Phenergan or Zofran may also be given for nausea if needed. Pain Medicine and anesthesia cause constipation sometimes and it is best to get off narcotics as soon as possible. You will also need to add fiber to your diet, such as fruit and vegetables. In some instances, you may have to take an over the counter laxative. I f you aren’t on a blood thinner you can start tapering off your pain medicine by taking an anti-inflammatory medicine along with a Tylenol to help with your pain and swelling. If you don’t normally take an anti-inflammatory you may take 1-2 Advil (Ibuprofen) with 1 Tylenol or 1or 2 Aleve (Naprosyn) with one Tylenol twice a day.
Driving: You may drive after your first post op visit if you are not taking narcotic pain medication, and you have good control of your arm.
Returning to Work: You should be able to resume desk work and light activity in 2-4 weeks, and more strenuous activity in 6-8 weeks. Job duties and extent of the surgery will dictate when you return to work.
Return to Office: You will have a return appointment in 2 weeks following surgery for an assessment of your post-operative condition. This will need to be on a Monday or Thursday. Call 205-783-5900 to make an appointment.
Physical Therapy: You should start your exercises the day after surgery when you are fully awake. Most patients prefer to do Dr. Bramlett’s at home exercise program that he has developed. Icing with the GameReady ice machine will help with pain after all exercises.
Antibiotics Information
A joint replacement reacts much like a heart valve replacement to bacteria circulation within the blood stream.
It is required that you have an antibiotic before you have any dental/oral procedures for life.
You cannot have any dental work until 3 months after your surgery.
We can call in a prescription or your dentist can do this for you.
The antibiotic protocol for implant prophylaxis follows:
Amoxicillin 2.0 grams, taken orally one hour before procedure.
For amoxicillin/penicillin-allergic patients (one RX):
Clindamycin Adults, 600 mg given orally one hour before procedure;
Cephalexin or cefadroxil: Adults, 2.0 grams orally one hour before procedure
Azithromycin or clarithromycin: Adults 500 mg orally one hour before procedure.
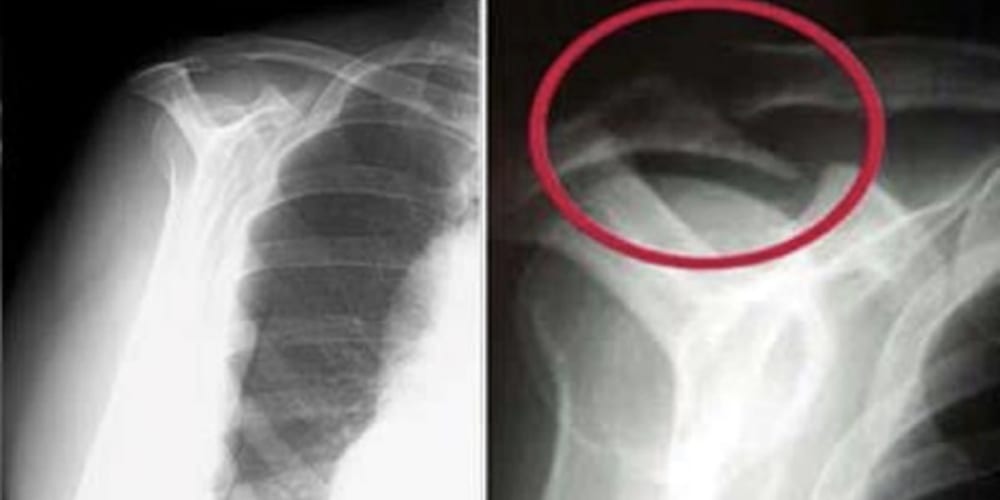
(Left) Normal outlet view x-ray. (Right) Abnormal outlet view showing a large bone spur causing impingement on the rotator cuff.
- Magnetic resonance imaging (MRI) and ultrasound. These studies can create better images of soft tissues like the rotator cuff tendons. They can show fluid or inflammation in the bursa and rotator cuff. In some cases, partial tearing of the rotator cuff will be seen.
Treatment
The goal of treatment is to reduce pain and restore function. In planning your treatment, your doctor will consider your age, activity level, and general health.
Nonsurgical Treatment
In most cases, initial treatment is nonsurgical. Although nonsurgical treatment may take several weeks to months, many patients experience a gradual improvement and return to function.
Rest. Your doctor may suggest rest and activity modification, such as avoiding overhead activities.
Non-steroidal anti-inflammatory medicines. Drugs like ibuprofen and naproxen reduce pain and swelling.
Physical therapy. A physical therapist will initially focus on restoring normal motion to your shoulder. Stretching exercises to improve range of motion are very helpful. If you have difficulty reaching behind your back, you may have developed tightness of the posterior capsule of the shoulder (capsule refers to the inner lining of the shoulder and posterior refers to the back of the shoulder). Specific stretching of the posterior capsule can be very effective in relieving pain in the shoulder.
Once your pain is improving, your therapist can start you on a strengthening program for the rotator cuff muscles.
Steroid injection. If rest, medications, and physical therapy do not relieve your pain, an injection of a local anesthetic and a cortisone preparation may be helpful. Cortisone is a very effective anti-inflammatory medicine. Injecting it into the bursa beneath the acromion can relieve pain.
may relieve painful symptoms.
Surgical Treatment
When nonsurgical treatment does not relieve pain, your doctor may recommend surgery.
The goal of surgery is to create more space for the rotator cuff. To do this, your doctor will remove the inflamed portion of the bursa. He or she may also perform an anterior acromioplasty, in which part of the acromion is removed. This is also known as a subacromial decompression. These procedures can be performed using either an arthroscopic or open technique.
Arthroscopic technique. In arthroscopy, thin surgical instruments are inserted into two or three small puncture wounds around your shoulder. Your doctor examines your shoulder through a fiberoptic scope connected to a television camera. He or she guides the small instruments using a video monitor, and removes bone and soft tissue. In most cases, the front edge of the acromion is removed along with some of the bursal tissue.
Your surgeon may also treat other conditions present in the shoulder at the time of surgery. These can include arthritis between the clavicle (collarbone) and the acromion (acromioclavicular arthritis), inflammation of the biceps tendon (biceps tendonitis), or a partial rotator cuff tear.
Open surgical technique. In open surgery, your doctor will make a small incision in the front of your shoulder. This allows your doctor to see the acromion and rotator cuff directly.
Rehabilitation. After surgery, your arm may be placed in a sling for a short period of time. This allows for early healing. As soon as your comfort allows, your doctor will remove the sling to begin exercise and use of the arm.
Your doctor will provide a rehabilitation program based on your needs and the findings at surgery. This will include exercises to regain range of motion of the shoulder and strength of the arm. It typically takes 2 to 4 months to achieve complete relief of pain, but it may take up to a year.

